IV Moderate Sedation for General Dentists: Safety, Protocol, and Building Patient Trust
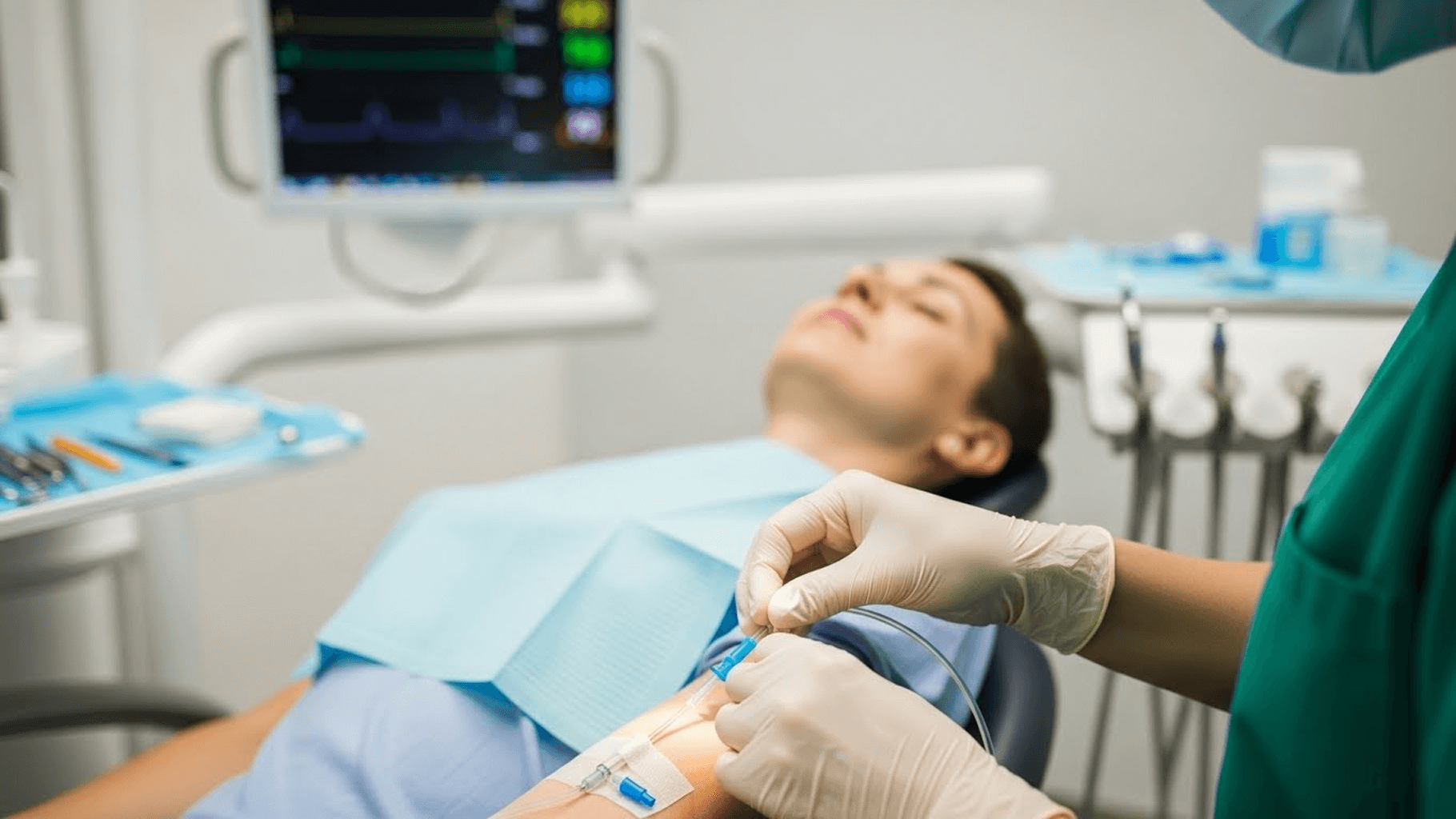
IV moderate sedation is one of the most practice-transforming skills a general dentist can acquire. When performed with proper training and protocol, it allows clinicians to treat a broader range of patients — including those with dental anxiety, complex medical histories, or lengthy procedures — in a controlled, office-based environment.
But effective sedation goes far beyond pharmacology. It demands clinical preparation, sound judgment, continuous monitoring, and a team trained to respond. This article breaks down the core pillars of safe IV moderate sedation for general dentists — and explains why mastering this skill is also one of the most powerful ways to build lasting patient trust.
What Is IV Moderate Sedation in Dentistry?
IV moderate sedation — also called parenteral conscious sedation — is a drug-induced depression of consciousness administered intravenously. The patient remains responsive to verbal commands and maintains independent airway function throughout the procedure.
Unlike general anesthesia, moderate sedation does not require intubation or an anesthesiologist on-site. This makes it a viable option for qualified general dentists who have completed a state-approved IV sedation certification course meeting the 2016 ADA Guidelines for Teaching Pain Control and Sedation to Dentists and Dental Students.
When implemented correctly in a dental practice, IV sedation reduces patient anxiety, improves cooperation during complex procedures, and significantly expands the range of cases a general dentist can handle in-house — including wisdom teeth extractions, multiple restorations, and implant placements.
The Four Pillars of Safe IV Sedation
Safe IV moderate sedation in a dental office is built on four interconnected pillars. Weakness in any one of them creates risk.
1. Patient Evaluation and Selection
Every sedation case begins before the patient sits in the chair. A thorough pre-operative evaluation is non-negotiable. This includes reviewing the patient's complete medical history, current medications, ASA physical status classification, NPO (fasting) status, and identifying any contraindications to sedation.
High-risk patients — including those with severe cardiovascular disease, COPD, obstructive sleep apnea, or obesity — require additional scrutiny. Knowing when not to sedate a patient is just as important as knowing how.
2. Accurate Drug Dosing and Titration
IV moderate sedation typically involves a combination of a benzodiazepine (most commonly midazolam) and an opioid analgesic (such as fentanyl), titrated incrementally based on patient response. The goal is to reach a comfortable, cooperative state — not oversedation.
Understanding the pharmacokinetics of each drug, how they interact, and how to recognize early signs of oversedation is a core competency that comes only from structured didactic training followed by supervised clinical experience with live patients.
3. Continuous Monitoring
During IV sedation, continuous monitoring is mandatory. Standard monitoring includes pulse oximetry, capnography (end-tidal CO₂), blood pressure, ECG, and respiratory rate. The combination of oximetry and capnography allows early detection of respiratory depression before oxygen saturation drops.
A trained dental assistant dedicated exclusively to monitoring is a critical component of a safe sedation team. This is not a one-person procedure.
4. Emergency Preparedness
Every dental office offering IV sedation must be equipped and prepared for emergencies. This means maintaining a fully stocked emergency kit including reversal agents (flumazenil for benzodiazepines, naloxone for opioids), a functional AED, oxygen delivery system, and a team current in ACLS (Advanced Cardiovascular Life Support).
Regular emergency simulations — not just annual reviews — are what separate prepared teams from unprepared ones.
How IV Sedation Training Builds Patient Trust
Patients are remarkably perceptive. They notice when a clinician is confident, prepared, and communicative — and they notice when something feels off.
One of the most consistent findings in dental sedation research is that patient trust is directly tied to clinician demeanor and perceived competence. When a dentist has been properly trained in IV sedation and routinely performs it, that confidence is visible. It shows in how the team moves, how questions are answered in the consultation, and how the environment is set up before the patient arrives.
The Consultation Conversation
Before any IV sedation case, a structured patient consultation is essential. This conversation should cover what to expect during and after sedation, informed consent (in plain language, not just a form), post-operative care instructions, and who to call with questions or concerns.
Dentists trained in IV sedation approach this conversation differently than those who have only read about it. Experience breeds clarity. Clarity builds trust.
Transparency About Safety Protocols
Patients considering sedation often have a specific concern: What if something goes wrong? The most effective answer is not reassurance — it's specifics. Being able to walk a patient through your monitoring setup, your emergency protocol, and your team's training credentials is a far more powerful trust-builder than a general statement about safety.
What IV Sedation Certification Requires
To legally offer IV moderate sedation in most states, general dentists must complete a certification course that meets the 2016 ADA guidelines. Core requirements typically include:
60 hours of didactic training covering pharmacology, airway management, patient monitoring, and emergency response
Minimum of 20 supervised live-patient IV sedation cases
Current ACLS certification
Successful demonstration of clinical competency signed off by the course director
State-specific permit application after course completion
The specific permit requirements vary by state. Some states require additional supervised cases, office inspections, or periodic recertification. Dentists should verify their state dental board requirements before enrolling in a course.
Common Questions About IV Sedation in Dental Offices
Can a general dentist legally administer IV moderate sedation?
Yes — in most U.S. states, a general dentist can legally administer IV moderate sedation after completing a state-approved certification course and obtaining the appropriate permit from their state dental board. Requirements vary by state, so verifying local regulations before enrolling is always recommended.
How long does it take to become certified in IV sedation?
Most IV sedation certification programs take between 4 and 6 months to complete. The timeline includes online didactic training (typically 35–60 hours) followed by an intensive hands-on clinical portion with live patients. Some programs are structured around weekends to minimize time away from the practice.
How much does IV sedation increase practice revenue?
Adding IV sedation to a dental practice typically allows dentists to bring in procedures they previously referred out — including complex extractions, implant placements, and multi-quadrant treatment sessions. Sedation also commands a separate fee (typically $400–$900 per case), and patients who are comfortable with sedation tend to accept larger treatment plans. The revenue impact is significant and begins within the first months of implementation.
What's the difference between IV moderate sedation and deep sedation?
Under IV moderate sedation, the patient remains conscious, responsive to verbal commands, and breathing independently. Deep sedation involves a deeper level of CNS depression where the patient may not respond purposefully and may require airway support. Deep sedation requires additional training and, in most states, a separate permit. Western Surgical and Sedation's training focuses on IV moderate sedation — the most commonly used level in general dental practice.







Related Articles
Related reading
Explore articles connected to surgical training, IV moderate sedation, and real world clinical decision making, selected to support dentists applying advanced care in daily practice.



